Simple Urine Test Detects Urothelial Cancers in Lynch Syndrome Patients
By LabMedica International staff writers
Posted on 24 Nov 2021
Lynch Syndrome (LS) is an inherited genetic disorder that carries a high risk of cancer. LS is caused by mutations affecting MLH1, MSH2, MSH6 or PMS2 genes. More than one in 300 people have LS but most do not know it and that is equivalent to more than 2,300 new cases every year in the UK.Posted on 24 Nov 2021
LS or hereditary nonpolyposis cancer patients are at high risk of bowel and endometrial cancers. The risk of urothelial cancer is less well recognized, with a lifetime risk of up to 28.5%, depending on which gene is involved. This means that those LS patients who have an underlying defect in the MSH2 gene are more than ten times as likely to get a potentially curable cancer in their urinary tract as the general population.
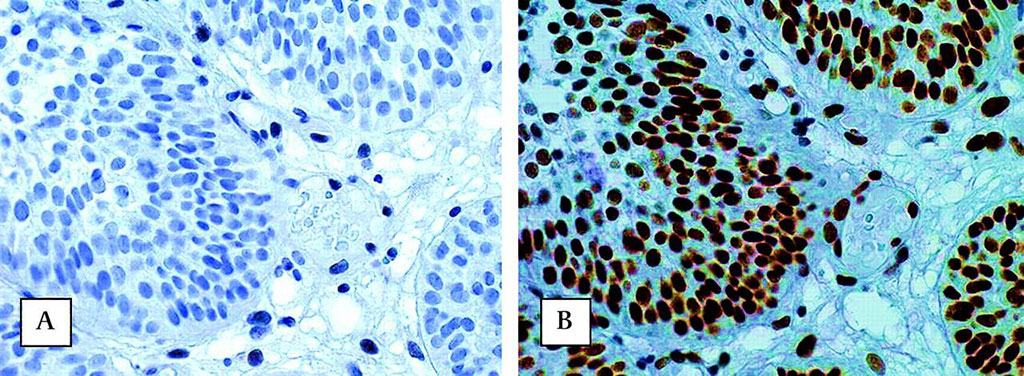
Image: Absence of nuclear immunohistochemical staining of MSH2 protein (A) and presence of MLH1 protein (B) in urothelial cell carcinoma of the urinary bladder of a patient carrying a germline MSH2 mutation. Observe the nuclear staining in stromal cells as an internal control (Photo courtesy of Radboud University Nijmegen Medical Centre)
Medical Scientists at Newcastle University (Newcastle upon Tyne, UK) redesigned the Newcastle MSI-Plus Assay. This has recently become the standard test in North East England to find people with LS among those diagnosed with bowel cancer. MSI, which stands for microsatellite instability, shows that an important DNA repair system is not working. Most LS patients are in this group. The test is being evaluated for national rollout.
To see if the test could be used for urothelial cancers as well as bowel cancer, the investigators tested blood and urine samples in a LS patient who had been diagnosed with urothelial cancer in the upper urinary tract. They tested the urine before and after surgery to remove the tumour. In a review of 10,243 urothelial cancers in England in 2018, they found that only 43 patients (0.4%) had undergone testing for genetic variants that could identify whether or not they carried the variants for LS. They estimated that around 2% of urothelial cancers are in people with the LS genetic mutations and at least 5% should be tested to identify LS cases, so there is an urgent need to improve screening for this disease.
Sir John Burn, MB BS, MD, Professor of Clinical Genetics and the presenter of the study, said, “Dying cells within the human body shed small fragments of DNA into the surrounding tissues and circulation. These fragments are known as cell-free DNA and can be extracted from urine. LS is caused by inherited changes that affect the cells’ ability to repair DNA damage. As a result, almost all cancers that develop within individuals with LS have a characteristic pattern of errors called microsatellite instability. Microsatellites are regions of repetitive DNA that often change their length if not repaired correctly. Our test uses this ‘signature’ to identify DNA from tumour cells that are shedding into the urine.”
The author concluded their findings offer the potential to develop a cheap, easy and non-invasive way of screening LS patients for cancers of the bladder, kidney and ureter (the tube connecting the bladder with the kidneys). The study was presented on November 11, 2021 at the virtual National Cancer Research Institute Festival.
Related Links:
Newcastle University