Mutation Found in Families with Contradictory Blood Sugars
By LabMedica International staff writers
Posted on 01 Feb 2018
Insulinomatosis is a condition characterized by the occurrence of multicentric insulinomas, pancreatic neuroendocrine tumors with β-cell–like features causing hyperinsulinemic hypoglycemia.Posted on 01 Feb 2018
Insulinomatosis usually occurs sporadically, although it had also been described to occur in a familial setting in one single kindred where hyperinsulinemic hypoglycemia was paradoxically associated with a strong family history of diabetes mellitus. Due to the multicentric nature of the disease, patients with insulinomatosis have a significantly higher chance of persistent or recurrent disease post-surgery.
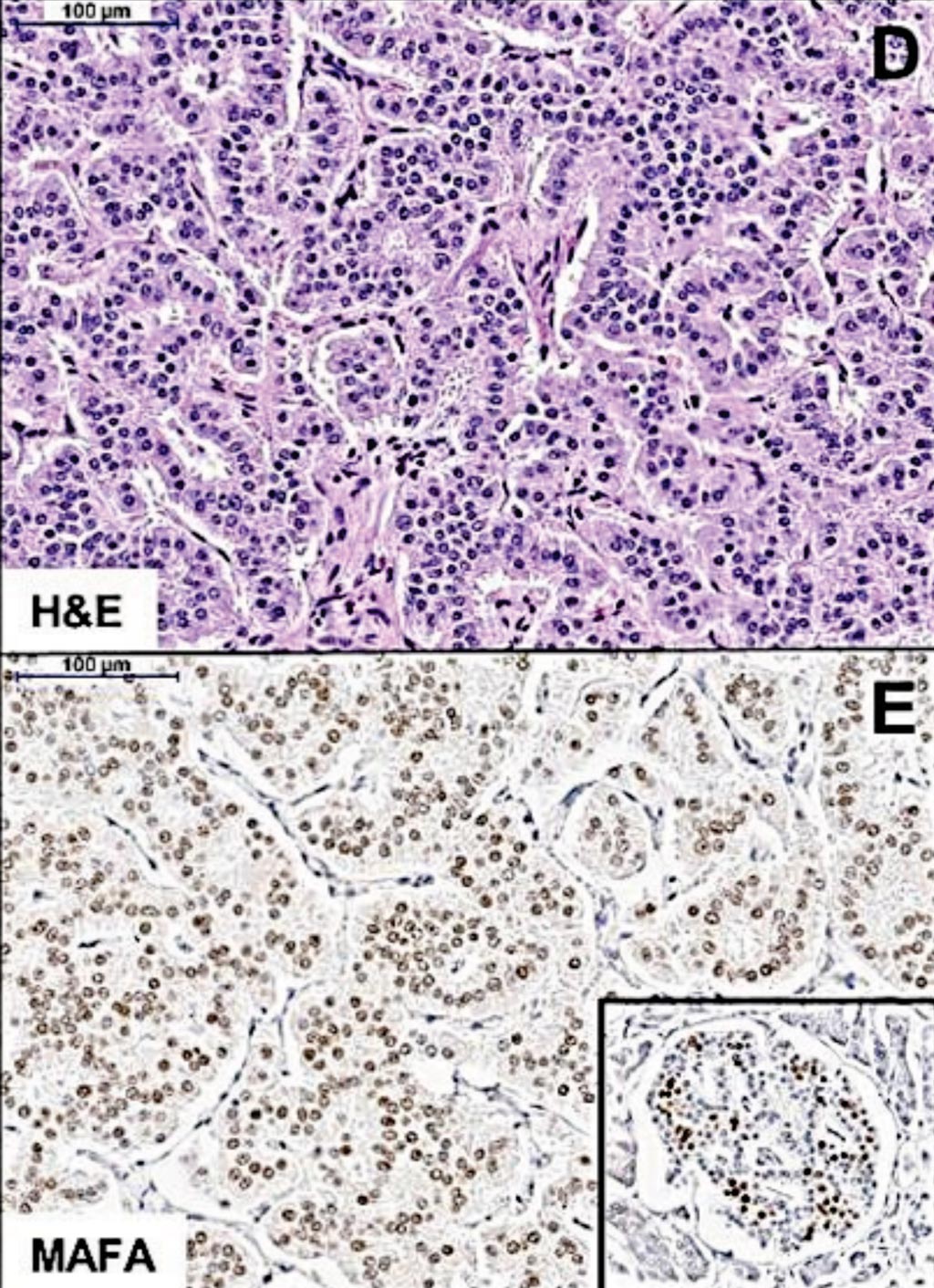
Image: Histopathology: (D) H&E staining showing the trabecular pattern of MAFA mutation-positive insulinomas. (E) Immunostaining shows diffuse MAFA expression in the tumor, at lower levels compared with the neighboring normal islets strongly expressing MAFA (Inset) (Photo courtesy of the Queen Mary University of London).
A collaborating group of international scientists working with those at the Queen Mary University of London (London, UK) recruited two families with autosomal dominant insulinomatosis and diabetes mellitus (36 subjects, 19 females), and nine patients with sporadic insulinomatosis (eight females). The two families in which some people have contradictory conditions due to high blood sugar and low blood sugar levels share a missense mutation. Both families contain members with diabetes and others with insulinomatosis, multiple pancreatic tumors that produce insulin and lower blood sugar levels.
The team performed immunohistochemistry on archival pancreatic tissue for neuroendocrine markers, Ki-67, and pancreatic hormones (insulin, gastrin, glucagon, and pancreatic polypeptide). Genomic DNA was extracted from peripheral blood leukocytes, saliva, or formalin-fixed archival tissue using commercially available kits. Other techniques employed by the scientists were protein mobility analysis, luciferase assays, and cycloheximide chase experiments. The quantitative polymerase chain reaction (qPCR) reactions were performed with MAFA-Myc, MAFA (endogenous), and GAPDH gene primers on a LightCycler 480 II.
The team sequenced the exomes of four affected people from the first family to find they all shared a missense mutation in the MAFA gene. When they tested all 25 members of that family for the mutation, they found an additional 14 members who were heterozygous for it and two who were homozygous. Seven of the heterozygous individuals had insulinomas, 10 had diabetes, and one was unaffected. The homozygous individuals had diabetes as well as congenital cataracts or glaucoma. Targeted sequencing of a second family with the same disease pattern likewise uncovered this missense MAFA mutation. Five individuals from this family with the mutation had insulinomatosis, one had diabetes, and two were not thought to be affected. In addition, three deceased family members, two with diabetes and one with insulinomatosis, were obligate carriers.
Donato Iacovazzo, MD, an endocrinologist and first author of the study, said, “We believe this gene defect is critical in the development of the disease and we are now performing further studies to determine how this defect can, on the one hand, impair the production of insulin to cause diabetes and on the other, cause insulinomas.” The study was published on January 16, 2018, in the journal Proceedings of the National Academy of Sciences.
Related Links:
Queen Mary University of London