Key Factors Signal Infection Risk in Alcoholic Hepatitis
By LabMedica International staff writers
Posted on 17 Aug 2021
Alcohol-associated hepatitis (AAH) is a severe form of liver injury with mortality as high as 30%-40% at 90 days. As a result of altered immune function in AAH, bacterial infections are common and are associated with poor outcomes.Posted on 17 Aug 2021
Severe cases of AAH are characterized by new onset jaundice. Infections are common in severe AAH, with approximately 25% of patients presenting with community-acquired infection and a similar percentage found to develop nosocomial infections. The high rates of sepsis observed in AAH may be explained by the impact of alcohol excess on the immune system.
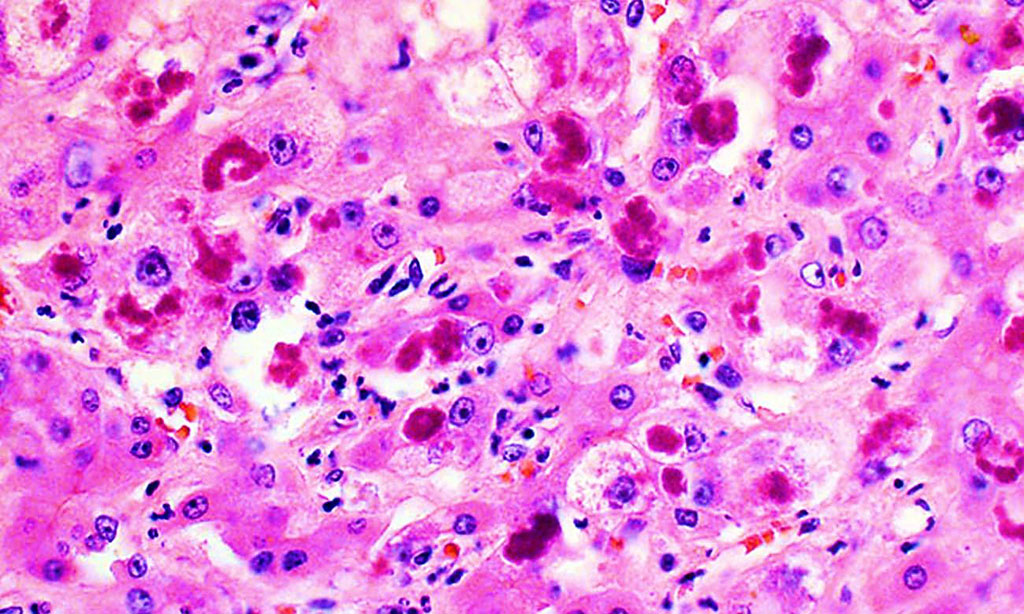
Image: Histopathology shows extensive liver cell damage resulting from alcoholic hepatitis (Photo courtesy of The Johns Hopkins University)
Gastroenterologists and their colleagues at the Mayo Clinic Rochester (Rochester, MN, USA) performed a retrospective study of consecutive patients admitted with a diagnosis of AAH at two independent tertiary centers from 1998 to 2018 (test cohort, n = 286) who developed infections following hospitalization. The cohort was 66% men, and the median age was 48 (range: 21-83) years. Corticosteroids were used in 32% of all patients with AAH.
Patients were diagnosed with AAH based on the clinical criteria and laboratory data including aspartate aminotransferase (AST) >50, aspartate aminotransferase/alanine aminotransferase (ALT) ratio >1.5, AST/ALT <400 IU/L, and serum bilirubin (total) >3.0 mg/dL. When the diagnosis of AAH remained unclear, a liver biopsy was obtained for confirmation. Types of infection were categorized as a urinary tract infection (UTI), bloodstream infection (BSI), pneumonia (PNA), spontaneous bacterial peritonitis (SBP), and Clostridium difficile (C. diff).
The scientists reported that the overall incidence of infection in the cohort was 36% (n = 102). They then excluded those who presented to the hospital with community-acquired infection, which was 12% (n = 34) of patients. The most common sources of infection at presentation were UTI (12), BSI (10), lower respiratory (6), SBP (3), and C. diff (3), and the most commonly identified organisms included Escherichia coli (8) and Staphylococcus aureus (6). Of those who developed an infection while hospitalized (31/286), the most common infection sources included lower respiratory tract infections (10), BSI (7), SBP (6), UTI (6), and C. diff (2).
Daniel Penrice, MD, a co-author of the study, said, “Our hope is that future studies can evaluate whether targeted prophylactic antibiotics for patients at high-risk for infection can improve survival. Our prediction model can likely be strengthened by the inclusion of novel biomarkers such as circulating serum bacterial DNA, endotoxin, or bacterial 16S ribosomal DNA.”
The authors concluded that in this multicenter cohort study of patients hospitalized with AAH, MELD score, ascites, WBC count, and use of corticosteroids were identified as significant predictors of the development of bacterial infection. They created a novel predictive equation that may be used to aid in the identification of patients with AAH at high risk of infection. The study was published on July 28, 2021 in the journal Hepatology Communications.
Related Links:
Mayo Clinic Rochester