White Blood Cell Help Define Pediatric Urinary Tract Infections
By LabMedica International staff writers
Posted on 25 Mar 2021
Urinary tract infections account for up to 7% of fevers in children up to 24 months old and are a common driver of hospital emergency room visits. These bacterial infections in infants and toddlers can be difficult to diagnose because their symptoms are similar to other fever-causing conditions.Posted on 25 Mar 2021
If a diagnosis is delayed, a UTI can develop into a serious infection that can cause lasting consequences. For example, UTI-related kidney scarring has been linked with hypertension and chronic kidney disease later in life. To diagnose a UTI, doctors must culture a urine sample and wait for it to grow telltale bacteria in a petri dish containing nutrients. However, this process can take up to two days, delaying treatment.
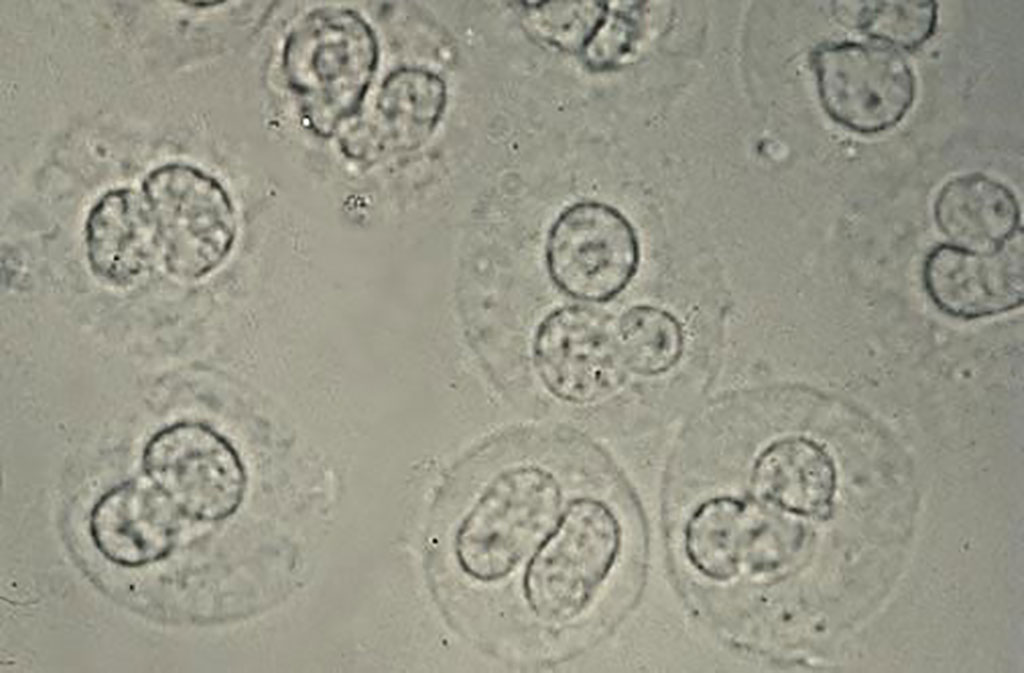
Image: White blood cells in the urine of a patient with bacteriuria pyuria, a urinary tract infection. The cells have lobed nuclei and refractile cytoplasmic granules (Photo courtesy of University of Utah Medical School).
Pediatricians and their colleagues at UT Southwestern Medical Center (Dallas, TX, USA) carried out a retrospective cross-sectional study of children less than 24 months of age evaluated in the emergency department for suspected UTI with paired urinalysis and urine culture during a 6-year period. The primary outcome was positive urine culture result and culture thresholds. Test characteristics for microscopic pyuria cut points and positive leukocyte esterase (LE) were calculated across three urine specific gravity groups: low <1.011, moderate 1.011 to 1.020, and high >1.020.
The team reported that of the total 24,171 patients analyzed, urine culture result was positive in 2,003 (8.3%). They used the urine's specific gravity and found that optimal white blood cell (WBC) cutoffs per high-power field (HPF) were three (positive likelihood ratio [LR+] 10.5; negative likelihood ratio [LR−] 0.12) at low, six (LR+ 12; LR− 0.14) at moderate, and eight (LR+ 11.1; LR− 0.35) at high urine concentrations. Likelihood ratios for small positive LE from low to high urine concentrations (LR+ 25.2, LR− 0.12; LR+ 33.1, LR− 0.15; LR+ 37.6, LR− 0.41) remained excellent.
Shahid Nadeem, MD, an assistant professor of pediatrics and lead author of the study, said, “For each of these concentration groups, leukocyte esterase remained constant, suggesting that it's a good trigger for analyzing urine for the presence of white blood cells. Knowing how many white blood cells tend to be present in urine samples at different concentrations in children with UTIs could help physicians start treating these infections before they receive urine culture results, giving relief to patients and their parents and preventing complications.”
The authors concluded that the optimal pyuria cut point in predicting positive urine culture results changes with urine concentration in young children. Pyuria thresholds of three WBCs per HPF at low urine concentrations whereas eight WBCs per HPF at high urine concentrations have optimal predictive value for UTI. Positive LE is a strong predictor of UTI regardless of urine concentration. The study was published in the February 2021 issue of the journal Pediatrics.
Related Links:
UT Southwestern Medical Center




.jpg)