New Official Guideline Summarizes Advances in Fungal Infections Diagnosis
By LabMedica International staff writers
Posted on 09 Sep 2019
An official clinical guideline on laboratory diagnosis of fungal infections in pulmonary and critical care medicine was released in a recent publication.Posted on 09 Sep 2019
Timely diagnosis of fungal infections, which are of increasing incidence and importance in immunocompromised and immunocompetent patients, relies on appropriate use of laboratory testing in susceptible patients.
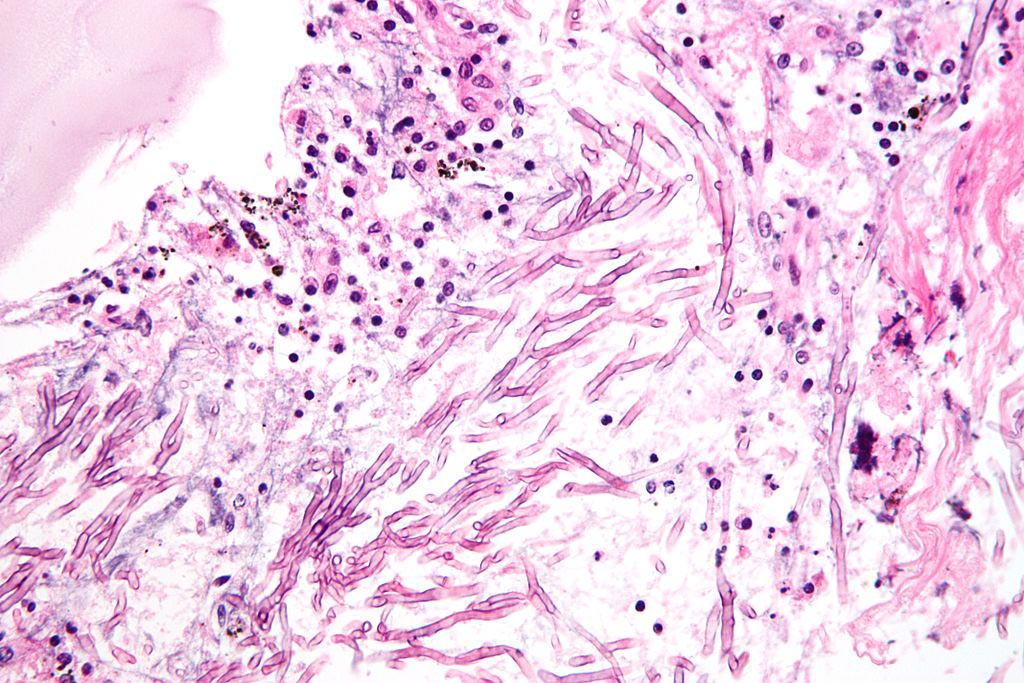
Image: A micrograph showing a mycosis (aspergillosis). The Aspergillus (which is spaghetti-like) is seen in the center and surrounded by inflammatory cells and necrotic debris (Photo courtesy of Wikimedia Commons).
In this regard, a panel of 11 experts in pulmonary and critical care, infectious disease, and invasive procedures appointed by the American Thoracic Society (New York, NY, USA) conducted a systematic review of medical studies on diagnosing fungal infections that had been published from 1980 to April 2016. The resulting official guideline covered the diagnosis of invasive pulmonary aspergillosis, invasive candidiasis, and the three most common endemic mycoses: blastomycosis, coccidioidomycosis, and histoplasmosis.
In particular, the panel addressed four clinical questions that clinicians face when they care for patients with suspected fungal infections: 1) Is serum and/or bronchoalveolar lavage (BAL) galactomannan (GM) testing sufficiently accurate to guide therapeutic decisions in place of histopathology and/or fungal culture in patients with impaired immunity suspected of having invasive pulmonary aspergillosis (IPA)? 2) Should diagnosis of suspected aspergillus infections in severely immunocompromised patients be based on the application of polymerase chain reaction (PCR)? 3) In critically ill patients with suspected invasive candidiasis, is the (1→3)-β-D-glucan (BDG) assay alone sufficient for diagnostic decision-making? 4) Should diagnosis of the common endemic mycoses (i.e., histoplasmosis, blastomycosis, coccidioidomycosis) be based on serology and antigen testing?
The guideline included specific recommendations for dealing with these situations, stressing that rapid, accurate diagnosis of fungal infections relied on appropriate application of laboratory testing, including antigen testing, serological testing, and PCR-based assays.
“Our goal was to produce a concise evidence-based clinical practice guideline that will help clinicians use newer laboratory methods in diagnosis of these important infections,” said guideline co-chair Dr. Andrew H. Limper, professor of pulmonary medicine at the Mayo Clinic (Rochester, MN, USA). “This guideline summarizes the best available evidence on the use of common laboratory tests to diagnose invasive pulmonary aspergillosis, invasive candidiasis, as well as histoplasmosis, blastomycosis, and coccidioidomycosis.”
“As always, application of any guideline information must be integrated into the overall clinical context for an individual patient when confirming the diagnosis of invasive fungal infection,” said Dr. Limper.
The guideline was published in the September 1, 2019, issue of the Journal of Respiratory and Critical Care Medicine.
Related Links:
American Thoracic Society
Mayo Clinic




.jpg)