Glucocorticoid Use Associated with Serious Bacterial Blood Infection Risk
By LabMedica International staff writers
Posted on 21 Jun 2016
The risk of life-threatening blood infections by Staphylococcus aureus bacteria is more than doubled in users of systemic glucocorticoids compared with non-users and the risk escalates with increasing dose.Posted on 21 Jun 2016
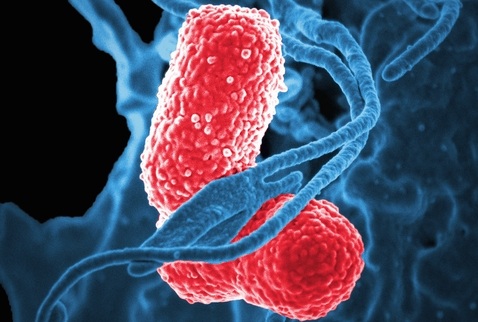
S. aureus is a bacterium that normally lives harmlessly on the skin, but occasionally it causes infection, which can be fatal if the bacteria enter the bloodstream. Glucocorticoids are potent immunosuppressive drugs when given through the mouth or by injection and are used for treatment of many different medical conditions.
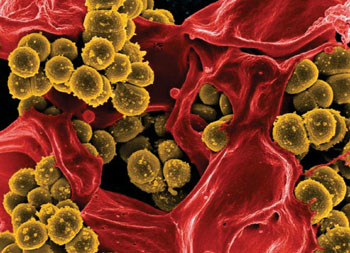
Image: A colorized scanning electron micrograph (SEM) of a strain of Staphylococcus aureus bacteria enmeshed within the pseudopodia of a red-colored human white blood cell (WBC) (Photo courtesy of the National Institute of Allergy and Infectious Diseases).
Scientists at the Aalborg University Hospitals (Denmark) and at Aarhus University Hospital (Denmark) and their German colleagues analyzed records of nearly 30,000 people using Danish medical registries over a 12-year period. The team investigated the risk of infection while taking into account duration of glucocorticoid use, 90-day cumulative dose, and specific groups of patients who are very frequently prescribed glucocorticoids.
The users of systemic glucocorticoids experienced a 2.5 times increased risk of S. aureus infection acquired outside of a hospital, as compared with non-users. The risk of infection rose gradually with increasing cumulative dose; compared with non-users. Patients with a 90-day cumulative dose of less than or equal to 150 mg were 2.4 times more at risk, rising to as high as 6.3 times greater risk among those with a cumulative dose of more than 1,000 mg. Among patients with connective tissue disease or chronic pulmonary disease, the risk of S. aureus blood infection was most pronounced in long-term users of glucocorticoids, whereas the risk was highest for new users among cancer patients.
Jesper Smit, MD, the lead author of the study, said, “Our study provides evidence that use of systemic glucocorticoids is associated with considerable risk of S. aureus blood infection, particularly among persons receiving high-dose therapy. These results may serve as a reminder for clinicians to weigh carefully the elevated risk against the potential beneficial effect of glucocorticoid therapy. This is especially pertinent in patients who are already vulnerable to infection.” The study was published on June 8, 2016, in the journal Mayo Clinic Proceedings.
Related Links:
Aalborg University Hospitals
Aarhus University Hospital