Immune Signature Predicts Poor Outcome in Influenza Patients
By LabMedica International staff writers
Posted on 27 Feb 2014
A signature immune response has been identified that might help doctors identify which newly diagnosed influenza patients are most likely to develop severe symptoms and suffer poor outcomes.Posted on 27 Feb 2014
Children are an at-risk population for developing complications following influenza infection, but immunologic correlates of disease severity are not understood and it has been hypothesized that innate cellular immune responses at the site of infection would correlate with disease outcome.
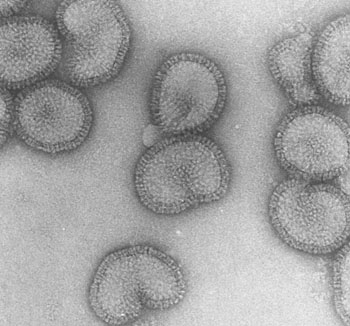
Image: Electron micrograph of influenza viruses (Photo courtesy of University of Saskatchewan).
Scientists at St. Jude Children’s Research Hospital (Memphis, TN, USA) conducted an observational cohort study with longitudinal sampling of peripheral and mucosal sites in 84 naturally influenza-infected individuals, including infants. Cellular responses, viral loads, and cytokines were quantified from nasal lavages and blood, and correlated to clinical severity. Sampling began when patients sought medical attention for influenza symptoms, and was repeated on days 3, 7, 10, and 28. Along with measuring levels of influenza virus in the nose and sinuses, researchers measured 42 cytokines and antibodies against circulating influenza viruses.
The testing showed children and adults were equally successful at eliminating the virus regardless of the subtype. In fact, based on cytokine levels in the blood, nose, and sinuses of patients, children mounted a more aggressive inflammatory response than adults. Adjusting for age and viral load, an innate immune profile characterized by increased nasal lavage monocyte chemotactic protein-3, interferon (IFN)-α2, and plasma interleukin 10 (IL-10) levels at enrollment predicted progression to severe disease. Increased plasma IL-10, monocyte chemotactic protein-3, and IL-6 levels predicted hospitalization.
Christine Oshansky, PhD, the senior author said, “The fact that the innate immune response was stronger in the airways of children than adults was a surprise. Previous studies using different measures reported that children mounted a weaker immune response. In this study, the hyperactive immune response diminished with age, but it may help explain why toddlers and infants are more likely to develop severe symptoms. Normal genetic variation might play a role in the innate immune response.” The study was published on February 15, 2014, in the American Journal of Respiratory and Critical Care Medicine.
Related Links:
St. Jude Children’s Research Hospital




.jpg)