Immature Natural Killer Cells Predict Relapse After Cord Blood Transplantation
By LabMedica International staff writers
Posted on 31 Dec 2019
Umbilical cord blood transplantation (CBT) has become an accepted alternative treatment of patients with hematologic cancers or other disorders. Many of the disadvantages of CBT, including limited numbers of total nucleated cells, have been dealt with in significant ways, leading to marked reductions in the time to hematopoietic cell recovery.Posted on 31 Dec 2019
Natural killer (NK) cells are highly heterogeneous, with vast phenotypic and functional diversity at the single-cell level. They are involved in the innate immune response against malignant and virus-infected cells. Although the kinetics of T- and B-cell subset recovery after CBT are well-described, much less is known about the recovery of CB-derived natural killer (NK) cells in the post-transplant setting.
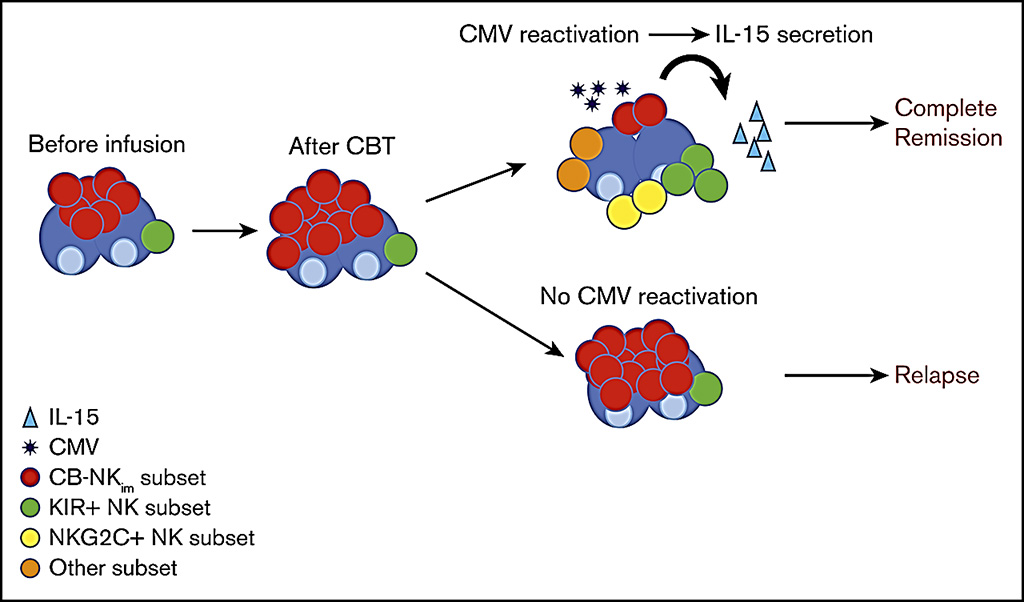
Image: Schematic diagram of how novel immature natural killer cell subpopulation predicts relapse after cord blood transplantation (CBT) (Photo courtesy of MD Anderson Cancer Center).
Stem transplantation specialists at The University of Texas MD Anderson Cancer Center (Houston, TX, USA) used high-dimensional mass cytometry and the metrics of NK cell diversity to study the NK cell repertoire in serial samples from 43 CBT recipients. A panel comprising 40 metal-tagged antibodies was used for the detailed characterization of NK cells. To assess NK cell cytotoxicity, the team co-cultured NK cells with 51Cr-labeled K562 targets at multiple E:T ratios (20:1, 10:1, 5:1, 1:1); cytotoxicity was measured by target release of 51Cr.
Total RNA was collected from five million NK cells per donor and pooled libraries were sequenced (50-bp paired-end reads generated with the HiSeq 2500 (Illumina, San Diego, CA, USA). Data were acquired on a Helios mass cytometer (Fluidigm, South San Francisco, CA, USA) and fluorescence cytometry data were acquired on BD LSRFortessa X-20 (BD Biosciences, San Jose, CA, USA).
The investigators reported that a higher-diversity index based on single-cell combinatorial phenotypes was significantly associated with a lower risk for relapse after CBT. Cytomegalovirus reactivation was a major factor in the development of a more diverse NK repertoire after CBT. They identified a group of patients whose CB-derived NK cells after transplantation possessed an immature phenotype (CB-NKim), characterized by poor effector function and a low diversity index. Frequencies of CB-NKim of 11.8% or higher during the early post-CBT recovery phase were highly predictive for relapse, a finding that was validated in a second independent cohort of 25 patients. They also showed that the maturation, diversity, and acquisition of effector function by CB-NKim early after CBT were driven by interleukin 15.
The authors concluded that their data indicated that the diversity of the NK cell repertoire after CBT contributes importantly to the risk for subsequent relapse. They suggest that the use of diversity metrics and high-dimensional mass cytometry may be useful tools in predicting clinical outcomes and informing the design of therapeutic strategies to prevent relapse after CBT. The study was published on December 10, 2019 in the journal Blood Advances.
Related Links:
The University of Texas MD Anderson Cancer Center
Illumina
Fluidigm
BD Biosciences