Acute Myeloid Leukemia Risk Predicted in Healthy Individuals
By LabMedica International staff writers
Posted on 26 Jul 2018
The incidence of acute myeloid leukemia (AML) increases with age and mortality exceeds 90% when diagnosed after age 65. Most cases arise without any detectable early symptoms and patients usually present with the acute complications of bone marrow failure.Posted on 26 Jul 2018
The onset of such de novo AML cases is typically preceded by the accumulation of somatic mutations in preleukemic hematopoietic stem and progenitor cells (HSPCs) that undergo clonal expansion. However, recurrent AML mutations also accumulate in HSPCs during ageing of healthy individuals who do not develop AML, a phenomenon referred to as age-related clonal hematopoiesis (ARCH).
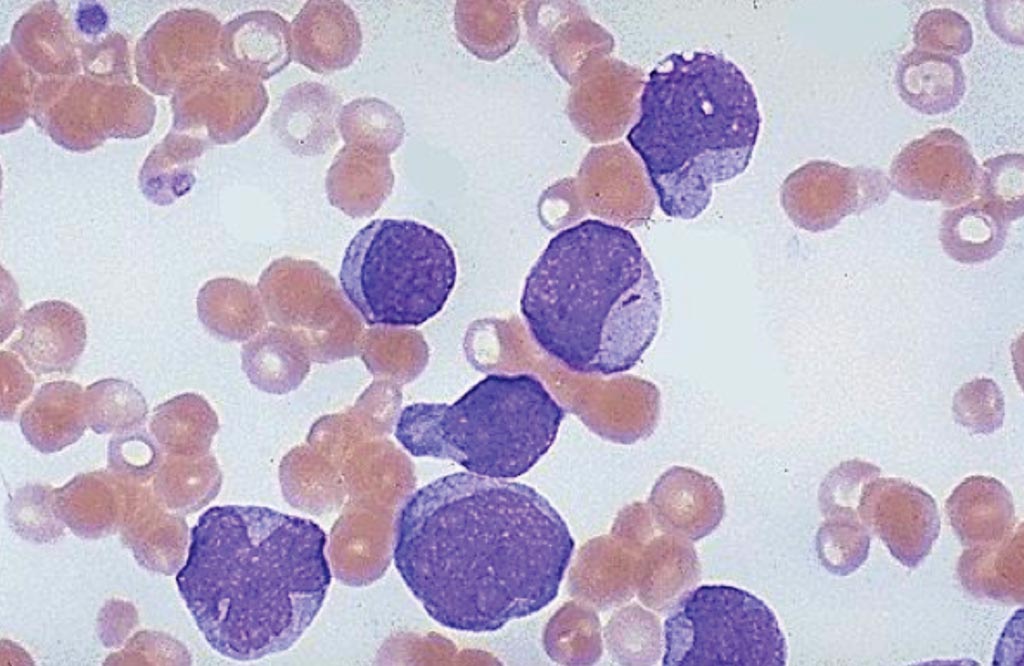
Image: A blood smear from a patient with acute myeloid leukemia showing very large, immature myeloblasts with many nucleoli. A distinctive feature of these blasts is a linear red \"Auer rod\" composed of crystallized granules (Photo courtesy of University of Utah Medical School).
An international team of scientists led by those at the Princess Margaret Cancer Centre (Toronto, ON, Canada) analyzed peripheral blood samples from 95 pre-AML cases and 414 age- and gender-matched controls. The pre-AML samples were obtained an average 6.3 years before diagnosis. The team validated their findings in an additional cohort of 29 cases and 262 controls. The team used use deep sequencing to analyze genes that are recurrently mutated in AML to distinguish between individuals who have a high risk of developing AML and those with benign ARCH.
The scientists reported that pre-AML cases were distinct from controls and had more mutations per sample, higher variant allele frequencies, indicating greater clonal expansion, and showed enrichment of mutations in specific genes. Genetic parameters were used to derive a model that accurately predicted AML-free survival. In the combined discovery and validation cohorts, 73.4% percent of the pre-AML cases had ARCH, while 36.7% of the controls did. In both groups, DNMTA3A and TET2 were commonly mutated. The group noted that they did not observe any canonical NPM2 mutations or FLT3-internal tandem duplication mutations, which they said was consistent with these mutations cropping up late in disease development.
The investigators also found that mutations in some genes conferred a greater risk of developing AML than others. For instance, mutations in DNMTA3A and TET2 confer a low risk of AML progression, while mutations in TP53 and U2F1 gave a much higher risk of disease progression. The scientist also developed a predictive test for AML into which they then folded additional data from patients' electronic health records. This test could predict AML six to 12 months before diagnosis with a sensitivity of 25.7% and a specificity of 98.2%.
George S. Vassiliou, FRCPath, MRCP, PhD, a cancer research senior fellow and a senior co-author of the study, said, “We hope to build on these findings to develop robust screening tests for identifying those at risk and drive research into how to prevent or stall progression towards AML.” The study was published on July 9, 2018, in the journal Nature.
Related Links:
Princess Margaret Cancer Centre