Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
Posted on 07 May 2026
Pancreatic cancer remains one of the hardest malignancies to treat because tumors are embedded within a dense microenvironment that shapes growth and therapy response. Standard laboratory models often miss the complex interplay among cancer, stromal, vascular, and immune compartments, limiting predictive value for drug testing. Understanding how scar-like stroma drives resistance is a priority for improving outcomes. A new study shows a patient‑derived tumor‑on‑a‑chip that recapitulates these interactions and enables longitudinal assessment of treatment response.
At UTHealth Houston’s McGovern Medical School (Houston, TX, USA), investigators developed a patient‑derived tumor‑on‑a‑chip system that recreates the pancreatic tumor microenvironment ex vivo. The platform combines three‑dimensional tumor organoids grown from consenting patients’ pancreatic tumor and blood samples with blood vessel, stromal, and immune cells integrated on a microfluidic chip. The device allows controlled fluid flow to mimic blood circulation, enabling continuous observation of cellular interactions and therapeutic responses over time.
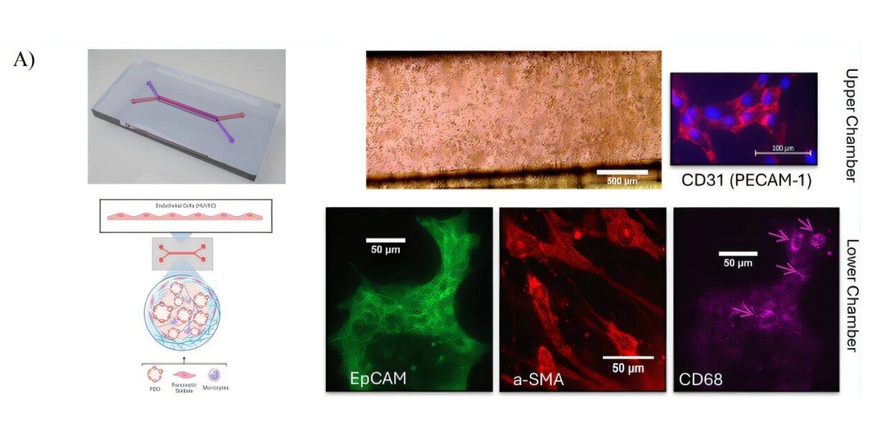
Within this microphysiological model, researchers used imaging, molecular analysis, and drug‑response testing to evaluate tumor behavior. The chip closely mirrored features of human pancreatic tumors and reproduced interactions with the desmoplastic, scar‑like stroma that are frequently implicated in treatment failure. The system also allowed monitoring of tumor structural evolution and pharmacologic responses across time.
Targeting stromal components within the chip increased the effectiveness of standard chemotherapy in this setting, indicating a means to interrogate mechanisms of resistance in a controlled, patient‑derived context. The model further demonstrated potential for studying immune responses that are often difficult to capture with conventional in vitro systems. The study is published in Advanced Science.
Looking ahead, the team notes efforts to improve the platform’s scalability, reproducibility, and broader usability for research applications. Collectively, the work underscores a shift toward human‑relevant models that integrate patient‑derived organoids with organ‑on‑a‑chip engineering to better approximate disease biology and therapeutic performance.
“This study shows that we can faithfully recreate key features of human pancreatic tumors, including interactions with stromal and immune cells,” said Faraz Bishehsari, MD, Ph.D., director of the Gastroenterology Research Center at McGovern Medical School at UTHealth Houston. "The next step is making these systems more practical so they can be widely used in research and drug development."
Related Links
McGovern Medical School at UTHealth Houston




.jpg)