Ultrasound, Nanoparticles Help Diabetics Avoid the Needle
By LabMedica International staff writers
Posted on 05 Dec 2013
A new nanotechnology-based technique for regulating blood sugar in diabetics may give patients the ability to release insulin painlessly using a small ultrasound device, allowing them to go days between injections, instead of using needles to give themselves multiple insulin injections each day. Posted on 05 Dec 2013
The technique was developed by researchers from North Carolina (NC) State University (Raleigh, USA) and the University of North Carolina (UNC; Chapel Hill, USA). “This is hopefully a big step toward giving diabetics a more painless method of maintaining healthy blood sugar levels,” said Dr. Zhen Gu, senior author of an article on the research and an assistant professor in the joint biomedical engineering program at NC State and UNC-Chapel Hill.
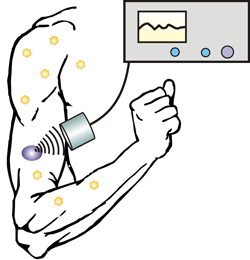
Image: A new technique allows diabetics to control insulin release with an injectable nano-network and portable ultrasound device (Photo courtesy of North Carolina State University).
The technique involves injecting biocompatible and biodegradable nanoparticles into a patient’s skin. The nanoparticles are comprised of poly(lactic-co-glycolic) acid (PLGA) and are filled with insulin. Each of the PLGA nanoparticles is given either a positively charged coating made of chitosan (a biocompatible substance typically found in shrimp shells), or a negatively charged coating comprised of alginate (a biocompatible substance typically found in seaweed). When the solution of coated nanoparticles is mixed together, the positively and negatively charged coatings are attracted to each other by electrostatic force to form a “nano-network.” Once injected into the subcutaneous layer of the skin, the network holds the nanoparticles together and prevents them from dispersing throughout the body.
The coated PLGA nanoparticles are also porous. Once in the body, the insulin begins to diffuse from the nanoparticles. But the bulk of the insulin does not wander far; it is suspended in a reservoir in the subcutaneous layer of the skin by the electrostatic force of the nano-network. This creates a dose of insulin that is merely waiting to be delivered into the bloodstream.
When a patient has type 1 or advanced type 2 diabetes, his or her body needs additional insulin, a hormone that transports glucose from the bloodstream into the body’s cells. These diabetes patients must inject insulin as needed to safeguard that their blood sugar levels are in the “normal” range. However, these injections can be painful. Using the new technology developed by Dr. Gu’s team, a diabetes patient does not have to inject a dose of insulin, as it is already there. Patients instead can use a small, hand-held device to apply focused ultrasound waves to the site of the nano-network, painlessly releasing the insulin from its de facto reservoir into the bloodstream.
The researchers theorized that the technology works because the ultrasound waves excite microscopic gas bubbles in the tissue, temporarily disrupting the network in the subcutaneous layer of the skin. That disruption moves the nanoparticles apart, relaxing the electrostatic force being exerted on the insulin in the reservoir. This allows the insulin to begin entering the bloodstream; a process accelerated by the effect of the ultrasound waves pushing on the insulin. “We know this technique works, and we think this is how it works, but we are still trying to determine the precise details,” noted Dr. Yun Jing, an assistant professor of mechanical engineering at NC State and co-corresponding author of the study.
When the ultrasound device is removed, the electrostatic force reestablishes itself and pushes the nanoparticles in the nano-network back together. The nanoparticles then diffuse more insulin, refilling the reservoir. “We’ve done proof-of-concept testing in laboratory mice with type 1 diabetes,” Dr. Gu stated. “We found that this technique achieves a quick release of insulin into the bloodstream, and that the nano-networks contain enough insulin to regulate blood glucose levels for up to 10 days.”
“When the insulin runs out, you have to inject a new nano-network,” said Dr. Jin Di, lead author of the paper and a PhD student in Dr. Gu’s research lab. “The previous nano-network is dissolved and fully absorbed into the body in a few weeks.”
“This advance will certainly give millions of people with diabetes worldwide hope that better days are ahead,” stated Dr. John Buse, director of UNC-Chapel Hill’s Diabetes Care Center and deputy director of UNC-Chapel Hill’s US National Institutes of Health (NIH; Bethesda, MD, USA) Clinical and Translational Sciences Award. “We must work to translate these exciting studies in the lab to clinical practice.”
The study was published online November 19, 2013, in the journal Advanced Healthcare Materials.
Related Links:
North Carolina State University
University of North Carolina