High-Throughput Isothermal HPV Test Validated
|
By LabMedica International staff writers Posted on 10 Mar 2020 |

Image: The AmpFire Multiplex Human papillomavirus (HPV) assay for real time fluorescent detection (Photo courtesy of AtilaBiosystems).
Human papillomavirus (HPV) is a viral infection that is passed between people through skin-to-skin contact. There are over 100 varieties of HPV, more than 40 of which are passed through sexual contact and can affect the genitals, mouth, or throat.
Some types of HPV are considered high risk because they can cause cancer. HPV testing detects the genetic material (DNA or messenger RNA) of high-risk HPV (hrHPV), primarily to screen for cervical cancer or to determine whether there is a risk of cervical cancer.
A large team of international scientists led by the Memorial Sloan Kettering Cancer Center (New York, NY, USA) performed an analytic validation of the AmpFire Multiplex HPV assays (AtilaBiosystems, Mountain View, CA, USA) on formalin-fixed, paraffin-embedded (FFPE) cervix/vulva and oropharynx diagnostic tissue samples. The AmpFire assay incorporates a novel isothermal multiplex amplification coupled with real-time fluorescent detection to detect and genotype 15 high-risk (HR) HPV genotypes.
The performance of the AmpFire assays in clinical samples was evaluated using 214 FFPE specimens. The international team also evaluated the Atila AmpFire HPV test comparing it to gold-standard testing, the Roche Cobas HPV and LinearArray tests (Risch-Rotkreuz, Switzerland). The team reported that the limits of detection determined by plasmids cloned with HPV genotype-specific sequences were two copies/reaction for HPV16, HPV18, and some HR HPV genotypes, and 20 copies/reaction for the remaining HR HPV genotypes.
The AmpFire assay failed in one clinical specimen for an invalid rate of 0.5%. The AmpFire assay detected HPV in clinical samples with positive percent agreements of 100% for HPV16, 100% for HPV18, and 94.7% for non-16/18 HR HPV, and 100% negative percent agreements for HPV16, HPV18, and non-16/18 HR HPV. Importantly, 53 of the FFPE clinical samples were biopsies of the oropharynx. In the USA, 70% of oropharyngeal cancers are HPV-related and fresh and preserved biopsy samples are frequently tested for HPV.
The authors concluded that qualitative detection agreement was obtained in their reproducibility study. In summary, the Atila AmpFire HPV assay demonstrated excellent analytic sensitivity and specificity for detection and genotyping of 15 HR HPV genotypes. Assay parameters of simple specimen processing, small sample size requirement, rapid turnaround time, and being near instrument-free render it well suited for HPV detection and genotyping in FFPE specimens. The study was published on January 21, 2020 in the Journal of Molecular Diagnostics
Related Links:
Memorial Sloan Kettering Cancer Center
AtilaBiosystems
Roche
Some types of HPV are considered high risk because they can cause cancer. HPV testing detects the genetic material (DNA or messenger RNA) of high-risk HPV (hrHPV), primarily to screen for cervical cancer or to determine whether there is a risk of cervical cancer.
A large team of international scientists led by the Memorial Sloan Kettering Cancer Center (New York, NY, USA) performed an analytic validation of the AmpFire Multiplex HPV assays (AtilaBiosystems, Mountain View, CA, USA) on formalin-fixed, paraffin-embedded (FFPE) cervix/vulva and oropharynx diagnostic tissue samples. The AmpFire assay incorporates a novel isothermal multiplex amplification coupled with real-time fluorescent detection to detect and genotype 15 high-risk (HR) HPV genotypes.
The performance of the AmpFire assays in clinical samples was evaluated using 214 FFPE specimens. The international team also evaluated the Atila AmpFire HPV test comparing it to gold-standard testing, the Roche Cobas HPV and LinearArray tests (Risch-Rotkreuz, Switzerland). The team reported that the limits of detection determined by plasmids cloned with HPV genotype-specific sequences were two copies/reaction for HPV16, HPV18, and some HR HPV genotypes, and 20 copies/reaction for the remaining HR HPV genotypes.
The AmpFire assay failed in one clinical specimen for an invalid rate of 0.5%. The AmpFire assay detected HPV in clinical samples with positive percent agreements of 100% for HPV16, 100% for HPV18, and 94.7% for non-16/18 HR HPV, and 100% negative percent agreements for HPV16, HPV18, and non-16/18 HR HPV. Importantly, 53 of the FFPE clinical samples were biopsies of the oropharynx. In the USA, 70% of oropharyngeal cancers are HPV-related and fresh and preserved biopsy samples are frequently tested for HPV.
The authors concluded that qualitative detection agreement was obtained in their reproducibility study. In summary, the Atila AmpFire HPV assay demonstrated excellent analytic sensitivity and specificity for detection and genotyping of 15 HR HPV genotypes. Assay parameters of simple specimen processing, small sample size requirement, rapid turnaround time, and being near instrument-free render it well suited for HPV detection and genotyping in FFPE specimens. The study was published on January 21, 2020 in the Journal of Molecular Diagnostics
Related Links:
Memorial Sloan Kettering Cancer Center
AtilaBiosystems
Roche
Latest Molecular Diagnostics News
- Urine Test to Revolutionize Lyme Disease Testing
- Simple Blood Test Could Enable First Quantitative Assessments for Future Cerebrovascular Disease
- New Genetic Testing Procedure Combined With Ultrasound Detects High Cardiovascular Risk
- Blood Samples Enhance B-Cell Lymphoma Diagnostics and Prognosis
- Blood Test Predicts Knee Osteoarthritis Eight Years Before Signs Appears On X-Rays
- Blood Test Accurately Predicts Lung Cancer Risk and Reduces Need for Scans
- Unique Autoantibody Signature to Help Diagnose Multiple Sclerosis Years before Symptom Onset
- Blood Test Could Detect HPV-Associated Cancers 10 Years before Clinical Diagnosis
- Low-Cost Point-Of-Care Diagnostic to Expand Access to STI Testing
- 18-Gene Urine Test for Prostate Cancer to Help Avoid Unnecessary Biopsies
- Urine-Based Test Detects Head and Neck Cancer
- Blood-Based Test Detects and Monitors Aggressive Small Cell Lung Cancer
- Blood-Based Machine Learning Assay Noninvasively Detects Ovarian Cancer
- Simple PCR Assay Accurately Differentiates Between Small Cell Lung Cancer Subtypes
- Revolutionary T-Cell Analysis Approach Enables Cancer Early Detection
- Single Genetic Test to Accelerate Diagnoses for Rare Developmental Disorders
Channels
Clinical Chemistry
view channel
3D Printed Point-Of-Care Mass Spectrometer Outperforms State-Of-The-Art Models
Mass spectrometry is a precise technique for identifying the chemical components of a sample and has significant potential for monitoring chronic illness health states, such as measuring hormone levels... Read more.jpg)
POC Biomedical Test Spins Water Droplet Using Sound Waves for Cancer Detection
Exosomes, tiny cellular bioparticles carrying a specific set of proteins, lipids, and genetic materials, play a crucial role in cell communication and hold promise for non-invasive diagnostics.... Read more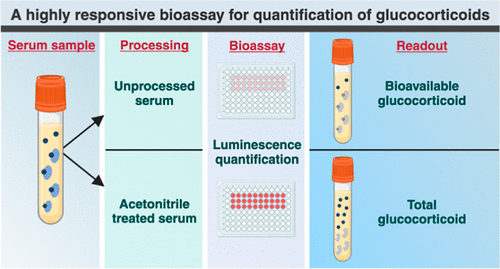
Highly Reliable Cell-Based Assay Enables Accurate Diagnosis of Endocrine Diseases
The conventional methods for measuring free cortisol, the body's stress hormone, from blood or saliva are quite demanding and require sample processing. The most common method, therefore, involves collecting... Read moreHematology
view channel
Next Generation Instrument Screens for Hemoglobin Disorders in Newborns
Hemoglobinopathies, the most widespread inherited conditions globally, affect about 7% of the population as carriers, with 2.7% of newborns being born with these conditions. The spectrum of clinical manifestations... Read more
First 4-in-1 Nucleic Acid Test for Arbovirus Screening to Reduce Risk of Transfusion-Transmitted Infections
Arboviruses represent an emerging global health threat, exacerbated by climate change and increased international travel that is facilitating their spread across new regions. Chikungunya, dengue, West... Read more
POC Finger-Prick Blood Test Determines Risk of Neutropenic Sepsis in Patients Undergoing Chemotherapy
Neutropenia, a decrease in neutrophils (a type of white blood cell crucial for fighting infections), is a frequent side effect of certain cancer treatments. This condition elevates the risk of infections,... Read more
First Affordable and Rapid Test for Beta Thalassemia Demonstrates 99% Diagnostic Accuracy
Hemoglobin disorders rank as some of the most prevalent monogenic diseases globally. Among various hemoglobin disorders, beta thalassemia, a hereditary blood disorder, affects about 1.5% of the world's... Read moreImmunology
view channel
Diagnostic Blood Test for Cellular Rejection after Organ Transplant Could Replace Surgical Biopsies
Transplanted organs constantly face the risk of being rejected by the recipient's immune system which differentiates self from non-self using T cells and B cells. T cells are commonly associated with acute... Read more
AI Tool Precisely Matches Cancer Drugs to Patients Using Information from Each Tumor Cell
Current strategies for matching cancer patients with specific treatments often depend on bulk sequencing of tumor DNA and RNA, which provides an average profile from all cells within a tumor sample.... Read more
Genetic Testing Combined With Personalized Drug Screening On Tumor Samples to Revolutionize Cancer Treatment
Cancer treatment typically adheres to a standard of care—established, statistically validated regimens that are effective for the majority of patients. However, the disease’s inherent variability means... Read moreMicrobiology
view channelEnhanced Rapid Syndromic Molecular Diagnostic Solution Detects Broad Range of Infectious Diseases
GenMark Diagnostics (Carlsbad, CA, USA), a member of the Roche Group (Basel, Switzerland), has rebranded its ePlex® system as the cobas eplex system. This rebranding under the globally renowned cobas name... Read more
Clinical Decision Support Software a Game-Changer in Antimicrobial Resistance Battle
Antimicrobial resistance (AMR) is a serious global public health concern that claims millions of lives every year. It primarily results from the inappropriate and excessive use of antibiotics, which reduces... Read more
New CE-Marked Hepatitis Assays to Help Diagnose Infections Earlier
According to the World Health Organization (WHO), an estimated 354 million individuals globally are afflicted with chronic hepatitis B or C. These viruses are the leading causes of liver cirrhosis, liver... Read more
1 Hour, Direct-From-Blood Multiplex PCR Test Identifies 95% of Sepsis-Causing Pathogens
Sepsis contributes to one in every three hospital deaths in the US, and globally, septic shock carries a mortality rate of 30-40%. Diagnosing sepsis early is challenging due to its non-specific symptoms... Read morePathology
view channel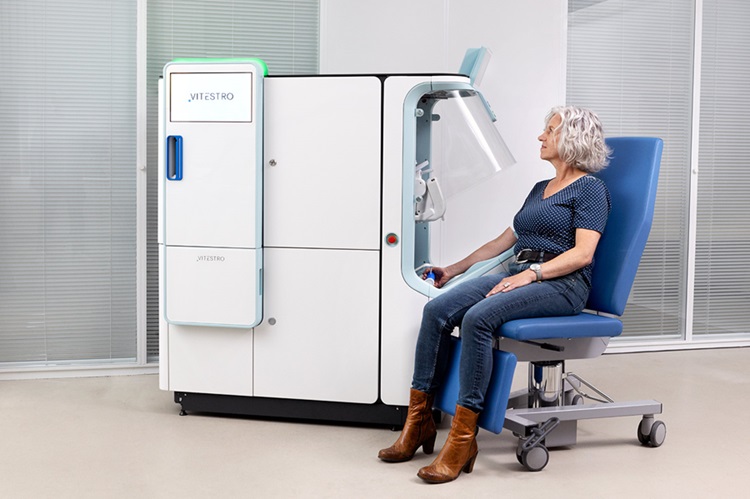
Robotic Blood Drawing Device to Revolutionize Sample Collection for Diagnostic Testing
Blood drawing is performed billions of times each year worldwide, playing a critical role in diagnostic procedures. Despite its importance, clinical laboratories are dealing with significant staff shortages,... Read more.jpg)
Use of DICOM Images for Pathology Diagnostics Marks Significant Step towards Standardization
Digital pathology is rapidly becoming a key aspect of modern healthcare, transforming the practice of pathology as laboratories worldwide adopt this advanced technology. Digital pathology systems allow... Read more
First of Its Kind Universal Tool to Revolutionize Sample Collection for Diagnostic Tests
The COVID pandemic has dramatically reshaped the perception of diagnostics. Post the pandemic, a groundbreaking device that combines sample collection and processing into a single, easy-to-use disposable... Read moreTechnology
view channel
New Diagnostic System Achieves PCR Testing Accuracy
While PCR tests are the gold standard of accuracy for virology testing, they come with limitations such as complexity, the need for skilled lab operators, and longer result times. They also require complex... Read more
DNA Biosensor Enables Early Diagnosis of Cervical Cancer
Molybdenum disulfide (MoS2), recognized for its potential to form two-dimensional nanosheets like graphene, is a material that's increasingly catching the eye of the scientific community.... Read more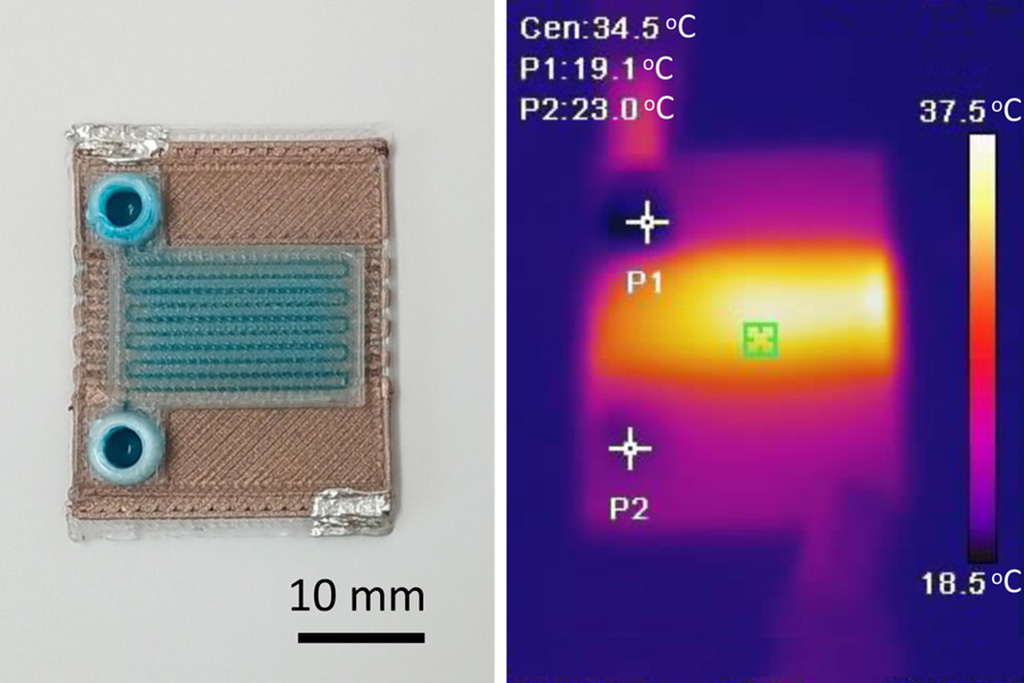
Self-Heating Microfluidic Devices Can Detect Diseases in Tiny Blood or Fluid Samples
Microfluidics, which are miniature devices that control the flow of liquids and facilitate chemical reactions, play a key role in disease detection from small samples of blood or other fluids.... Read more
Breakthrough in Diagnostic Technology Could Make On-The-Spot Testing Widely Accessible
Home testing gained significant importance during the COVID-19 pandemic, yet the availability of rapid tests is limited, and most of them can only drive one liquid across the strip, leading to continued... Read moreIndustry
view channel_1.jpg)
Thermo Fisher and Bio-Techne Enter Into Strategic Distribution Agreement for Europe
Thermo Fisher Scientific (Waltham, MA USA) has entered into a strategic distribution agreement with Bio-Techne Corporation (Minneapolis, MN, USA), resulting in a significant collaboration between two industry... Read more
ECCMID Congress Name Changes to ESCMID Global
Over the last few years, the European Society of Clinical Microbiology and Infectious Diseases (ESCMID, Basel, Switzerland) has evolved remarkably. The society is now stronger and broader than ever before... Read more