Gene Mutation Discovered in Blood Disorder Aplastic Anemia
|
By LabMedica International staff writers Posted on 07 Oct 2014 |
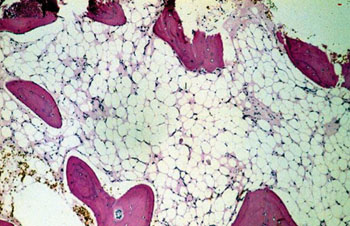
Image: Photomicrograph of a hypocellular bone marrow biopsy, due to lack of hematopoietic cells, from a patient with aplastic anemia (Photo courtesy of the Autonomous University of Zacatecas).
A gene mutation has been discovered that causes aplastic anemia, a serious blood disorder in which the bone marrow fails to produce normal amounts of blood cells.
Telomerase is a ribonucleoprotein enzyme that is necessary for overcoming telomere shortening in human germ and stem cells. Mutations in telomerase or other telomere maintenance proteins can lead to diseases characterized by depletion of hematopoietic stem cells and bone marrow failure.
Scientists at the Children's Hospital of Philadelphia (PA, USA) working with international colleagues investigated the family of a patient who had presented with severe thrombocytopenia and macrocytosis, and has been diagnosed with aplastic anemia. The family history includes other cases of bone marrow failure, as well as oral carcinoma and leukemia. Peripheral blood DNA was available from the patient, her parents, and maternal grandparents.
Whole exome sequencing was performed and the exonic regions were captured using SureSelect Human All Exon kit (Agilent; Santa Clara, CA, USA) and pair-end sequencing was carried out on HiSeq 2000 machines (Illumina; San Diego, CA, USA). A Telomere Flow-Fluorescence In Situ Hybridization (Flow-FISH) was performed and the subsequent flow cytometry was performed on a FACS CANTO II (BD Biosciences; San Jose, CA, USA). Other complimentary methodologies were also used to corroborate the initial findings.
The 18 year-old patient, her mother and maternal grandmother presented with bone marrow failure of varying severity, and their decreasing ages of presentation in successive generations suggested disease anticipation. The team found that that the mutation in Adrenocortical Dysplasia Homolog gene (ACD) alters the telomere-binding protein tripeptidyl peptidase 1 (TPP1), disrupting the interactions between telomere and telomerase. Without access to telomerase to help maintain telomeres, blood cells lose their structural integrity and die, resulting in bone marrow failure.
Hakon Hakonarson, MD, PhD, the director of the Center for Applied Genomics, and study co-leader, said, “Identifying this causal defect may help suggest future molecular-based treatments that bypass the gene defect and restore blood cell production. This improved understanding of the underlying molecular mechanisms may suggest new approaches to treating disorders such as aplastic anemia. For instance, investigators may identify other avenues for recruiting telomerase to telomeres to restore its protective function.” The study was published on September 9, 2014, in the journal Blood.
Related Links:
Children's Hospital of Philadelphia
Agilent
Illumina
Telomerase is a ribonucleoprotein enzyme that is necessary for overcoming telomere shortening in human germ and stem cells. Mutations in telomerase or other telomere maintenance proteins can lead to diseases characterized by depletion of hematopoietic stem cells and bone marrow failure.
Scientists at the Children's Hospital of Philadelphia (PA, USA) working with international colleagues investigated the family of a patient who had presented with severe thrombocytopenia and macrocytosis, and has been diagnosed with aplastic anemia. The family history includes other cases of bone marrow failure, as well as oral carcinoma and leukemia. Peripheral blood DNA was available from the patient, her parents, and maternal grandparents.
Whole exome sequencing was performed and the exonic regions were captured using SureSelect Human All Exon kit (Agilent; Santa Clara, CA, USA) and pair-end sequencing was carried out on HiSeq 2000 machines (Illumina; San Diego, CA, USA). A Telomere Flow-Fluorescence In Situ Hybridization (Flow-FISH) was performed and the subsequent flow cytometry was performed on a FACS CANTO II (BD Biosciences; San Jose, CA, USA). Other complimentary methodologies were also used to corroborate the initial findings.
The 18 year-old patient, her mother and maternal grandmother presented with bone marrow failure of varying severity, and their decreasing ages of presentation in successive generations suggested disease anticipation. The team found that that the mutation in Adrenocortical Dysplasia Homolog gene (ACD) alters the telomere-binding protein tripeptidyl peptidase 1 (TPP1), disrupting the interactions between telomere and telomerase. Without access to telomerase to help maintain telomeres, blood cells lose their structural integrity and die, resulting in bone marrow failure.
Hakon Hakonarson, MD, PhD, the director of the Center for Applied Genomics, and study co-leader, said, “Identifying this causal defect may help suggest future molecular-based treatments that bypass the gene defect and restore blood cell production. This improved understanding of the underlying molecular mechanisms may suggest new approaches to treating disorders such as aplastic anemia. For instance, investigators may identify other avenues for recruiting telomerase to telomeres to restore its protective function.” The study was published on September 9, 2014, in the journal Blood.
Related Links:
Children's Hospital of Philadelphia
Agilent
Illumina
Latest Molecular Diagnostics News
- Advanced Blood Test to Spot Alzheimer's Before Progression to Dementia
- Multi-Omic Noninvasive Urine-Based DNA Test to Improve Bladder Cancer Detection
- First of Its Kind NGS Assay for Precise Detection of BCR::ABL1 Fusion Gene to Enable Personalized Leukemia Treatment
- Urine Test to Revolutionize Lyme Disease Testing
- Simple Blood Test Could Enable First Quantitative Assessments for Future Cerebrovascular Disease
- New Genetic Testing Procedure Combined With Ultrasound Detects High Cardiovascular Risk
- Blood Samples Enhance B-Cell Lymphoma Diagnostics and Prognosis
- Blood Test Predicts Knee Osteoarthritis Eight Years Before Signs Appears On X-Rays
- Blood Test Accurately Predicts Lung Cancer Risk and Reduces Need for Scans
- Unique Autoantibody Signature to Help Diagnose Multiple Sclerosis Years before Symptom Onset
- Blood Test Could Detect HPV-Associated Cancers 10 Years before Clinical Diagnosis
- Low-Cost Point-Of-Care Diagnostic to Expand Access to STI Testing
- 18-Gene Urine Test for Prostate Cancer to Help Avoid Unnecessary Biopsies
- Urine-Based Test Detects Head and Neck Cancer
- Blood-Based Test Detects and Monitors Aggressive Small Cell Lung Cancer
- Blood-Based Machine Learning Assay Noninvasively Detects Ovarian Cancer
Channels
Clinical Chemistry
view channel
3D Printed Point-Of-Care Mass Spectrometer Outperforms State-Of-The-Art Models
Mass spectrometry is a precise technique for identifying the chemical components of a sample and has significant potential for monitoring chronic illness health states, such as measuring hormone levels... Read more.jpg)
POC Biomedical Test Spins Water Droplet Using Sound Waves for Cancer Detection
Exosomes, tiny cellular bioparticles carrying a specific set of proteins, lipids, and genetic materials, play a crucial role in cell communication and hold promise for non-invasive diagnostics.... Read more
Highly Reliable Cell-Based Assay Enables Accurate Diagnosis of Endocrine Diseases
The conventional methods for measuring free cortisol, the body's stress hormone, from blood or saliva are quite demanding and require sample processing. The most common method, therefore, involves collecting... Read moreMolecular Diagnostics
view channel
Advanced Blood Test to Spot Alzheimer's Before Progression to Dementia
Alzheimer’s disease is well known for its slow development over many years, which typically leads to treatment interventions only after the disease has advanced to stages where it may be nearly impossible... Read more
Multi-Omic Noninvasive Urine-Based DNA Test to Improve Bladder Cancer Detection
Hematuria, the presence of blood in urine, is commonly associated with bladder cancer and is its most frequent symptom. Current guidelines recommend referring patients with hematuria to urology for clinical... Read more.jpg)
First of Its Kind NGS Assay for Precise Detection of BCR::ABL1 Fusion Gene to Enable Personalized Leukemia Treatment
The BCR::ABL1 fusion gene plays a key role in the pathogenesis of several blood cancers, particularly chronic myeloid leukemia (CML). This gene results from a chromosomal translocation that causes constitutive... Read moreImmunology
view channel
Diagnostic Blood Test for Cellular Rejection after Organ Transplant Could Replace Surgical Biopsies
Transplanted organs constantly face the risk of being rejected by the recipient's immune system which differentiates self from non-self using T cells and B cells. T cells are commonly associated with acute... Read more
AI Tool Precisely Matches Cancer Drugs to Patients Using Information from Each Tumor Cell
Current strategies for matching cancer patients with specific treatments often depend on bulk sequencing of tumor DNA and RNA, which provides an average profile from all cells within a tumor sample.... Read more
Genetic Testing Combined With Personalized Drug Screening On Tumor Samples to Revolutionize Cancer Treatment
Cancer treatment typically adheres to a standard of care—established, statistically validated regimens that are effective for the majority of patients. However, the disease’s inherent variability means... Read moreMicrobiology
view channel
Integrated Solution Ushers New Era of Automated Tuberculosis Testing
Tuberculosis (TB) is responsible for 1.3 million deaths every year, positioning it as one of the top killers globally due to a single infectious agent. In 2022, around 10.6 million people were diagnosed... Read more
Automated Sepsis Test System Enables Rapid Diagnosis for Patients with Severe Bloodstream Infections
Sepsis affects up to 50 million people globally each year, with bacteraemia, formerly known as blood poisoning, being a major cause. In the United States alone, approximately two million individuals are... Read moreEnhanced Rapid Syndromic Molecular Diagnostic Solution Detects Broad Range of Infectious Diseases
GenMark Diagnostics (Carlsbad, CA, USA), a member of the Roche Group (Basel, Switzerland), has rebranded its ePlex® system as the cobas eplex system. This rebranding under the globally renowned cobas name... Read more
Clinical Decision Support Software a Game-Changer in Antimicrobial Resistance Battle
Antimicrobial resistance (AMR) is a serious global public health concern that claims millions of lives every year. It primarily results from the inappropriate and excessive use of antibiotics, which reduces... Read morePathology
view channel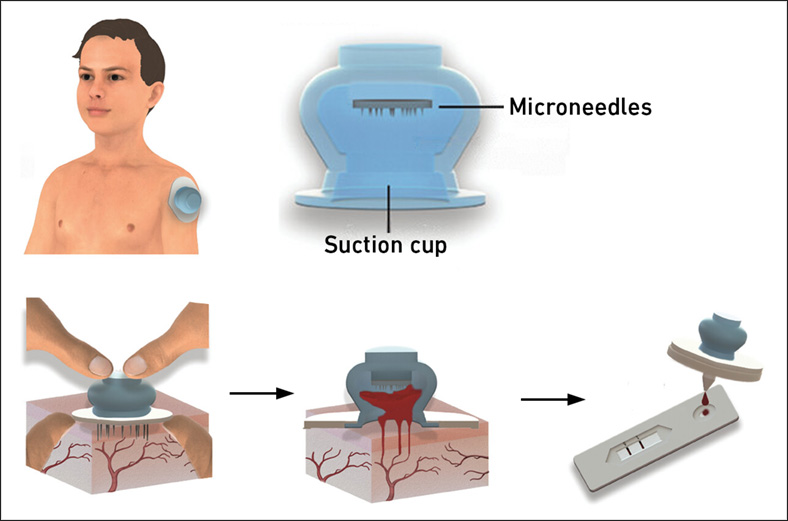
New Blood Test Device Modeled on Leeches to Help Diagnose Malaria
Many individuals have a fear of needles, making the experience of having blood drawn from their arm particularly distressing. An alternative method involves taking blood from the fingertip or earlobe,... Read more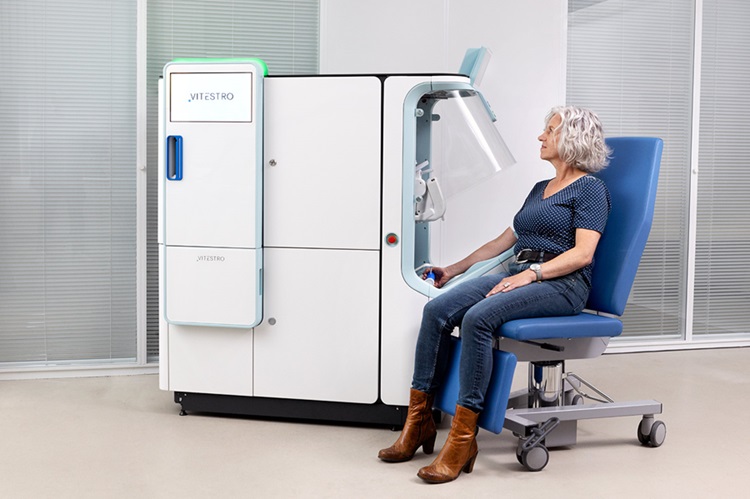
Robotic Blood Drawing Device to Revolutionize Sample Collection for Diagnostic Testing
Blood drawing is performed billions of times each year worldwide, playing a critical role in diagnostic procedures. Despite its importance, clinical laboratories are dealing with significant staff shortages,... Read more.jpg)
Use of DICOM Images for Pathology Diagnostics Marks Significant Step towards Standardization
Digital pathology is rapidly becoming a key aspect of modern healthcare, transforming the practice of pathology as laboratories worldwide adopt this advanced technology. Digital pathology systems allow... Read more
First of Its Kind Universal Tool to Revolutionize Sample Collection for Diagnostic Tests
The COVID pandemic has dramatically reshaped the perception of diagnostics. Post the pandemic, a groundbreaking device that combines sample collection and processing into a single, easy-to-use disposable... Read moreTechnology
view channel
New Diagnostic System Achieves PCR Testing Accuracy
While PCR tests are the gold standard of accuracy for virology testing, they come with limitations such as complexity, the need for skilled lab operators, and longer result times. They also require complex... Read more
DNA Biosensor Enables Early Diagnosis of Cervical Cancer
Molybdenum disulfide (MoS2), recognized for its potential to form two-dimensional nanosheets like graphene, is a material that's increasingly catching the eye of the scientific community.... Read more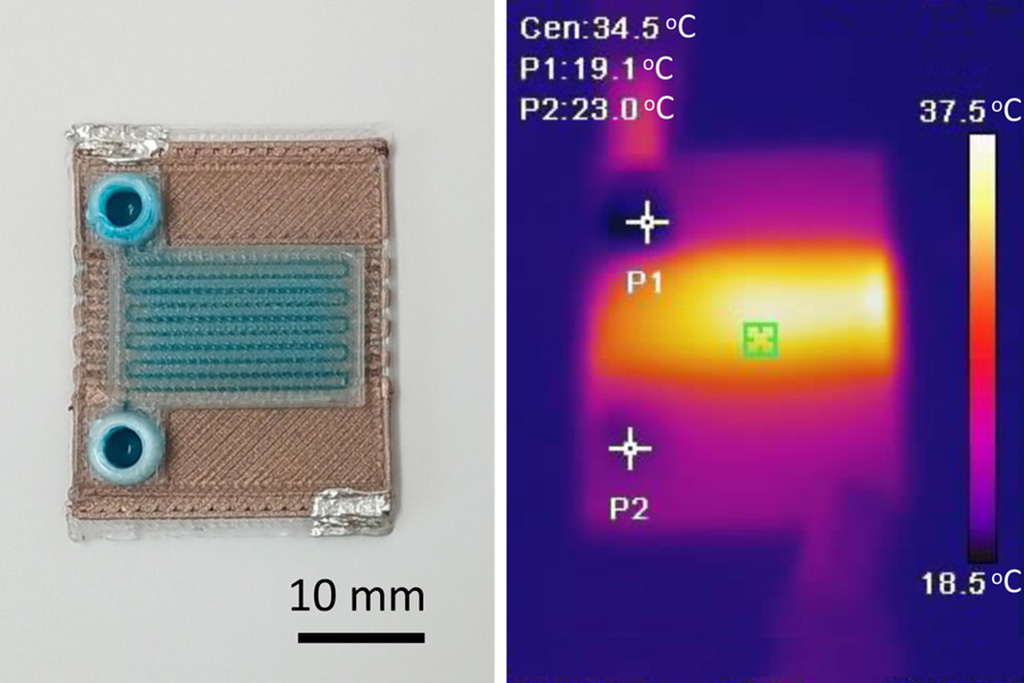
Self-Heating Microfluidic Devices Can Detect Diseases in Tiny Blood or Fluid Samples
Microfluidics, which are miniature devices that control the flow of liquids and facilitate chemical reactions, play a key role in disease detection from small samples of blood or other fluids.... Read more
Breakthrough in Diagnostic Technology Could Make On-The-Spot Testing Widely Accessible
Home testing gained significant importance during the COVID-19 pandemic, yet the availability of rapid tests is limited, and most of them can only drive one liquid across the strip, leading to continued... Read moreIndustry
view channel_1.jpg)
Thermo Fisher and Bio-Techne Enter Into Strategic Distribution Agreement for Europe
Thermo Fisher Scientific (Waltham, MA USA) has entered into a strategic distribution agreement with Bio-Techne Corporation (Minneapolis, MN, USA), resulting in a significant collaboration between two industry... Read more
ECCMID Congress Name Changes to ESCMID Global
Over the last few years, the European Society of Clinical Microbiology and Infectious Diseases (ESCMID, Basel, Switzerland) has evolved remarkably. The society is now stronger and broader than ever before... Read more